
Retrograde menstruation occurs when blood flows backwards into the pelvis instead of out of the vagina during menstruation. Retrograde menstruation is common, and occurs to some degree in most women who have their period. Despite this, some scientists believe that women with significant retrograde menstruation may be at increased risk for endometriosis.
It is thought that retrograde menstruation can deposit endometrial cells outside of the uterus, where they may grow and become problematic. However, not all research supports a role for retrograde menstruation in endometriosis.
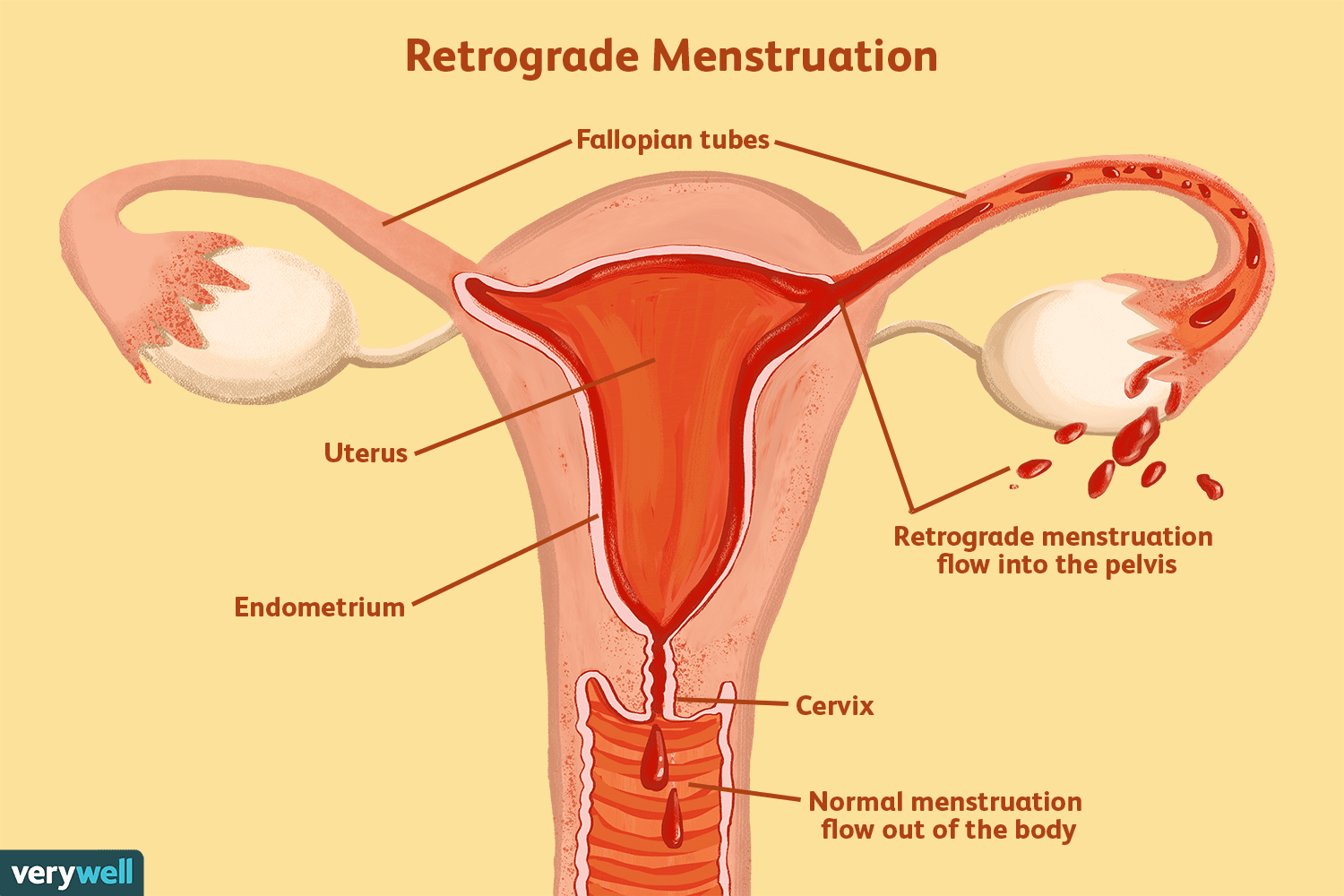
During retrograde menstruation, blood flows through the Fallopian tubes and out into the peritoneum rather than through the cervix and out the vagina. Women with retrograde menstruation often do not have any symptoms. The primary symptom associated with retrograde menstruation is pain during menstruation (dysmenorrhea). Unfortunately, this is a very non-specific symptom. Menstrual pain is also associated with many other conditions affecting reproductive health.
Most research about retrograde menstruation looks at it in the context of endometriosis. Therefore, there is very little research on the causes of retrograde menstruation. However, at least one study has demonstrated that women with blocked Fallopian tubes do not experience retrograde menstruation.
There is also basic research suggesting that having a smaller cervical opening may increase the risk of retrograde blood flow. Still, as research suggests that retrograde menstruation is extremely common among people who have a uterus, it should probably be considered a normal aspect of menstrual function.
Retrograde menstruation is only a medical concern if and when it leads to symptoms or other conditions, such as endometriosis.
Retrograde menstruation is not usually diagnosed as a condition on its own. It may be diagnosed in the context of endometriosis or pelvic pain evaluation. For example, retrograde menstruation might be diagnosed if healthcare providers do a laparoscopic examination of the pelvis during menstruation and they see blood.
Unfortunately, many women with endometriosis spend years in pain before they receive a diagnosis. Healthcare providers may attribute symptoms to the more common pain associated with periods; they may also consider painful periods to be normal. Discomfort during menstruation is common. However menstrual pain should not be disabling or affect a woman's ability to live her life. It is most helpful if healthcare providers are willing to look for causes other than assume it is due to primary dysmenorrhea. Endometriosis is thought to affect as many as 10% of women. It may not be easy to diagnose, but it's important to check for it when there are signs.
Retrograde menstruation is not treated unless it is causing other problems.
Treating retrograde menstruation usually involves prescribing hormones, or a hormonal IUD to reduce or eliminate menstrual flow.
A hysterectomy will also treat retrograde menstruation, but would only be used if there were another reason to remove the uterus.
Retrograde menstruation may sound scary, but remember that it isn't all that uncommon. It just means that when you get your period, some of the blood and tissue are flowing backward into your pelvis rather than out onto your pad, or into your cup or tampon. In general, retrograde menstruation is not something you need to worry about. If it is associated with other problems, such as endometriosis, those will be treated directly by your healthcare provider. Be sure to talk with your healthcare provider to discuss any extreme or unusual period pain.
Can You Do Anything to Prevent Endometriosis?