
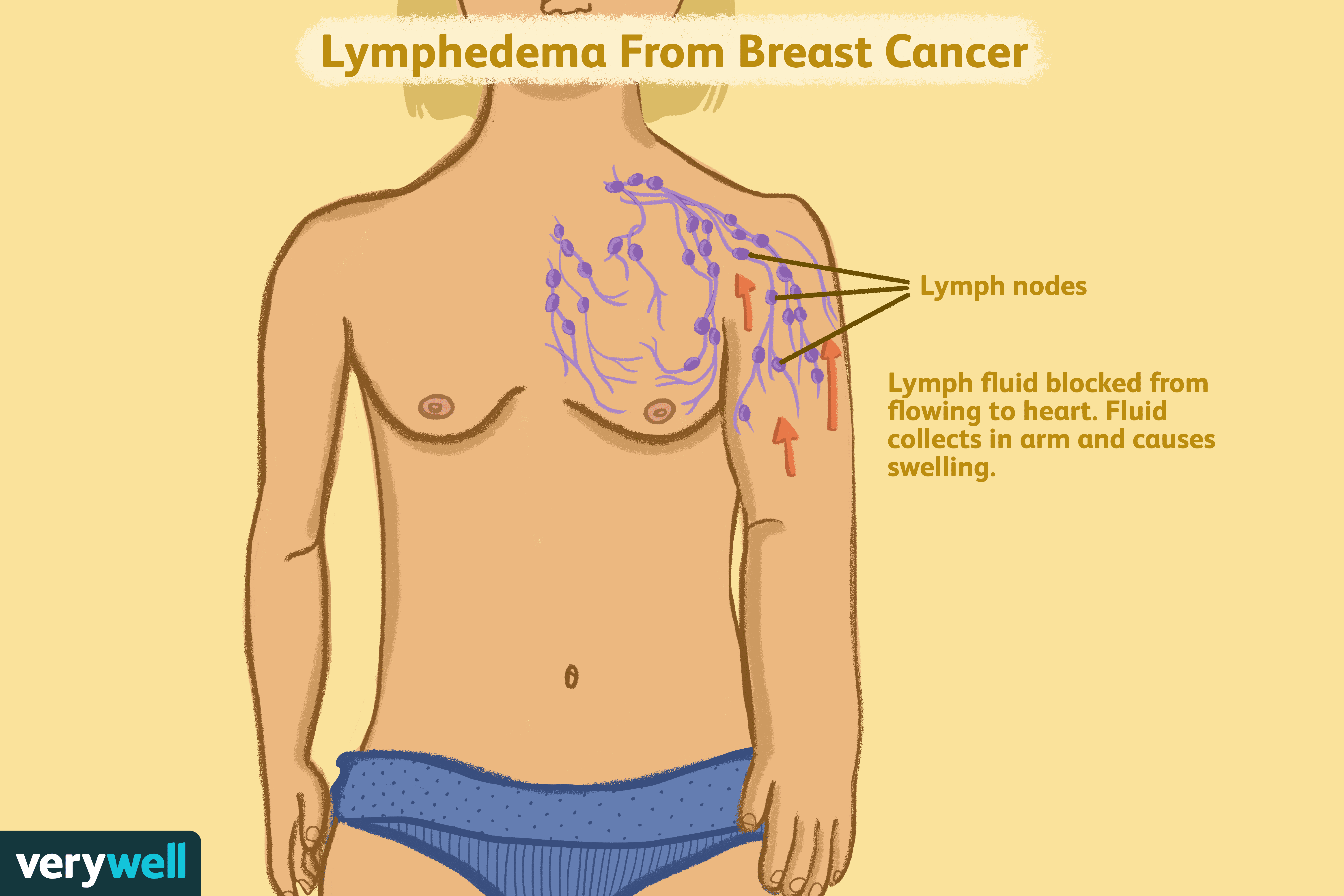
Lymphedema is a type of swelling that is commonly associated with cancer. In breast cancer, it typically affects the arm on the same side as the cancer. The swelling is the result of an accumulation of lymph—fluid that contains immune cells and proteins that flows throughout your body—that occurs when lymph nodes or lymph vessels become damaged or blocked. This is a common complication of breast surgery and radiation, but can also be due to a tumor itself.
In addition to swelling, lymphedema often brings pain, impeded flexibility, and other uncomfortable symptoms.
It is estimated that between 30 percent and 70 percent of women who have breast cancer develop lymphedema at some point during the disease course.
Sometimes lymphedema is temporary, occurring just after surgery and then resolving. Often, however, it is a chronic condition that waxes and wanes over the course of one's life, even after breast cancer has completely been cured. And rarely, lymphedema may occur decades after breast cancer surgery.
The main signs and symptoms of lymphedema include:
Untreated lymphedema can have serious consequences, including infections, skin ulcers (open sores that don't heal), and extreme swelling and thickening of the skin (elephantiasis).
The lymphatic system, through which your immune system rapidly delivers protective immune materials throughout the body, also includes lymph nodes that filter lymphatic fluid. Lymphedema occurs when the flow of lymphatic fluid through those vessels or nodes becomes impaired. The fluid can back up and enter into the nearby soft tissue, causing the characteristic swelling of lymphedema.
If you have breast cancer, surgery or radiation therapy can cause lymphedema to develop. And while it is less common, the disease itself can lead to lymphedema.
Breast cancer can result in lymphedema when:
Because breast cancer can spread to nearby lymph nodes, it is not uncommon for a breast cancer evaluation to include a lymph node biopsy. Biopsy or removal of lymph nodes in the chest or armpit increases the chances of developing lymphedema.
Lymph Node Status and Breast CancerLymphedema is diagnosed based on your physical examination and may involve some diagnostic testing as well. The arm swelling is usually evident, but it can be subtle. The diameter of the affected and unaffected arms can be compared with a tape measure, and these values may be recorded so your healthcare provider can see if you have any changes (improvement or worsening) over time. Most healthcare providers recommend that patients be screened for breast cancer-related lymphedema both during and after treatment.
If you have breast cancer, your healthcare providers might not do any additional testing to determine the cause of your lymphedema because breast cancer is often associated with this complication.
However, there are times when your medical team may be concerned that lymphedema is a sign of an infection or cancer extension. Congestive heart failure can also cause arm swelling, as can blood clots in the arm. Your medical team may need to rule out these health problems, and diagnostic tests can help clarify the cause of your arm swelling.
Imaging tests such as computed tomography (CT), ultrasound, or magnetic resonance imaging (MRI) scans can often identify masses or areas of infection.
Lymphatic scintigraphy involves the injection of a radioactive dye, followed by recorded images of the dye as it moves through the lymphatic system. This test can help identify areas of slow lymphatic flow or blockage.
Get our printable guide for your next healthcare provider's appointment to help you ask the right questions.

Symptoms of lymphedema, such as swelling and pain, can often be managed. The lymph nodes and lymphatic vessels cannot be repaired, but they may heal on their own.
Sometimes, physical pressure caused by a tumor can be relieved with surgery or radiation, but these treatments may worsen lymphedema and the main objective of these techniques is treating the tumor, not the lymphedema.
Lymphedema treatments include:
When you have lymphedema, it's important to avoid anything that might worsen your condition or cause complications. You will need to make a few adjustments to your daily life to avoid exacerbating your lymphedema.
Tips for coping include:
While some breast cancer survivors with lymphedema avoid air travel, researchers have found that air travel does not increase the risk developing lymphedema or worsen the condition.
Airplane travel can increase the risk of blood clots, and this risk is higher if you have or have had cancer. Lymphedema may also increase the risk of blood clots, so be sure to ask your healthcare provider if you should take any special precautions.
Lymphedema itself is not necessarily dangerous, but it can be uncomfortable, and there are a few complications associated with the condition. In some instances, lymphedema is the first sign that cancer is spreading, so it is important to let your healthcare provider know if you develop arm swelling for the first time or if your lymphedema worsens.