
Several genes have been linked to breast cancer, the most common of which are BRCA mutations (BRCA1 and BRCA2). To give you a sense of their significance, the overall lifetime risk of breast cancer in women without a BRCA mutation is around 12%. For those with such a mutation, the average lifetime risk of developing breast cancer varies between 40 to 70%. BRCA mutations increase the risk of several other types of cancer as well.
Since a BRCA mutation is such a significant risk factor, many women with a family history of the disease are encouraged to get genetic testing. Such testing is not routine and requires thoughtful consideration about potential next steps. The possibility of discovering a predisposition to breast cancer can be frightening, but surveillance and treatment can improve the long-term survival of people who have these mutations, and this should temper some of your fears.
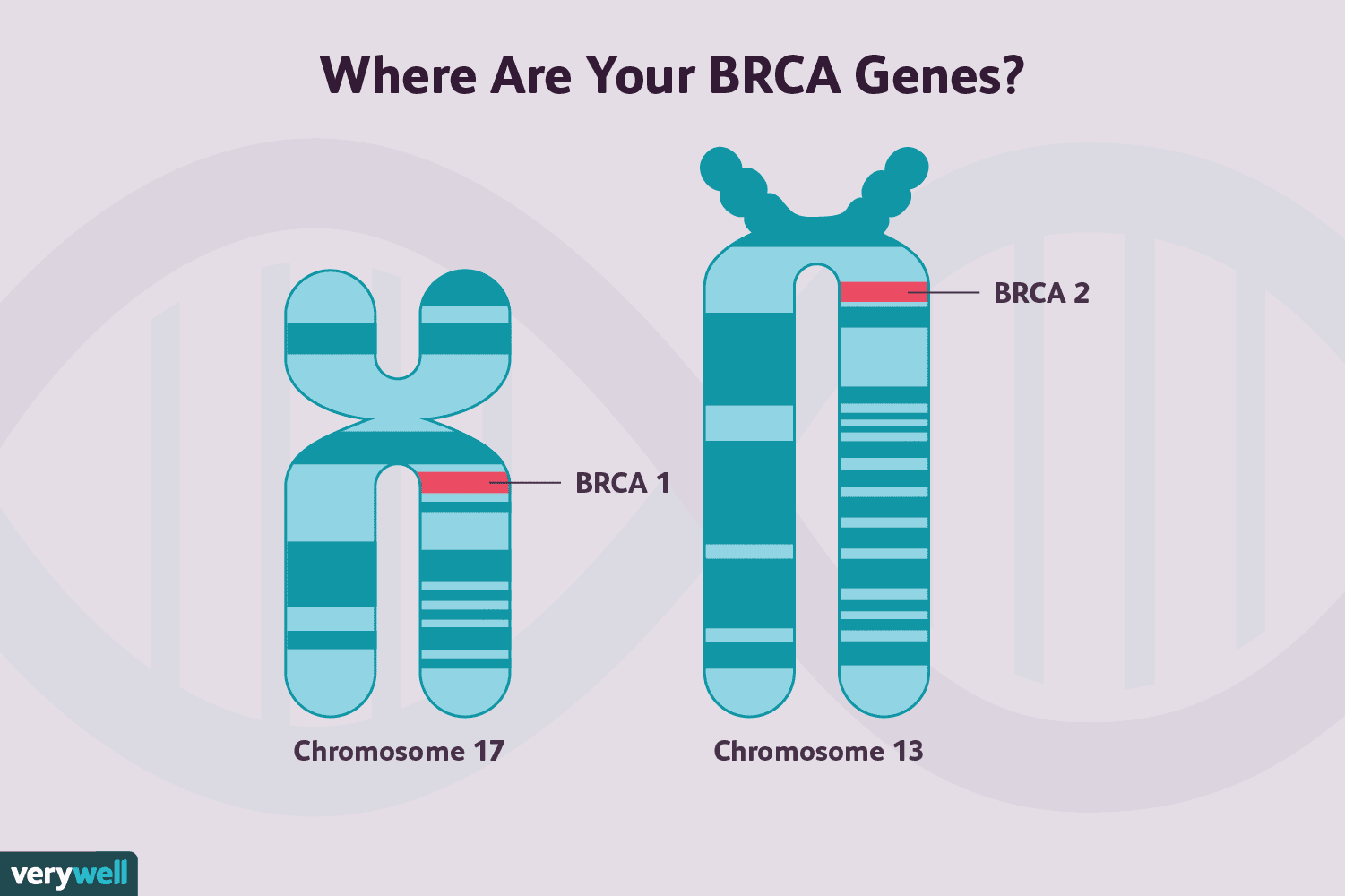
Genes, which are inside each cell in your body, are made of DNA molecules. They are a blueprint—coding for the proteins that your body builds. BRCA genes are normal genes that function as tumor suppressor genes. Each of your cells contains two copies of the BRCA1 gene and two copies of the BRCA2 gene (one copy of each from your mother and one copy from your father).
Normal BRCA genes code for proteins that prevent cancer growth, especially breast cancer and ovarian cancer. Specifically, these proteins are responsible for repairing cancer-causing damage to DNA in your cells.
You may hear some people refer to these by spelling out "B-R-C-A mutations" or by saying "braca mutations."
Understanding Oncogenesis, the Process That Leads to CancerMutations are genetic errors. BRCA gene mutations are autosomal dominant, meaning that having one copy of the abnormal gene impairs their normal anti-cancer effect.
It is far more common to have only one mutated BRCA gene (this is written as BRCA1/2) than two of them.
There are two ways for a person to have a BRCA gene mutation:
Having a BRCA mutation gives you a genetic predisposition to cancer, but it does not mean that you will definitely develop cancer.
BRCA mutations are associated with hereditary breast cancer, but not all hereditary breast cancers are due to BRCA mutations.
Overall, BRCA mutations account for 20 to 25% of hereditary breast cancers and 5 to 10% of breast cancers overall.
Hereditary breast cancers not related to BRCA mutations are referred to as non-BRCA familial breast cancer or BRCAX. Gene mutations that are linked to breast cancer include those in ATM CDH1, CHEK2, PALB2, PTEN, STK11, and TP53. There are likely others, and research is ongoing.
In those under age 40, about 10% of breast cancers are associated with being BRCA-positive, and after age 40, approximately 5% of breast cancers are associated with a BRCA gene mutation.
Familial Breast CancerThese mutations are associated with different tumor characteristics that can affect responsiveness to therapy. BRCA mutations tend to be associated with cancers that have a higher tumor grade, which is a measure of the aggressiveness of the tumor.
In addition, breast cancers in women with BRCA mutations (especially BRCA1) are less likely to have estrogen or progesterone receptors. These proteins on the surface of breast cancer cells cause tumors to grow when they bind with these hormones.
These mutations also are associated with breast cancer that is less likely to be HER2-positive.
Triple-negative breast cancers—which don't have HER2 receptors, estrogen receptors, or progesterone receptors—are more common in women with BRCA mutations than in women without the mutation. This means that medications that are effective for hormone receptor-positive and HER2-positive breast cancers are not usually effective for treating these cancers, which can make them more difficult to treat.
Breast cancers in women with BRCA mutations tend to respond better to neoadjuvant chemotherapy (chemotherapy prior to surgery) than those in women without these mutations.
Overall, genetic testing for breast cancer genes is not standard. However, it is often recommended for women who have a family history of breast cancer or who have personally had breast cancer at a young age.
While you might have medical indications for getting tested, this is an emotionally charged decision. You may be faced with major decisions if you test positive for BRCA genes or other breast cancer genes (often called non-BRCA gene mutations).
Many women want to get tested in every way possible, while others prefer to avoid knowing about their risks.
Considerations as you make a decision about getting tested:
Regardless of your decision about genetic testing, you need to get your recommended mammograms.
Keep in mind that a negative test result (no identified breast cancer genes) does not mean that you will not get breast cancer. Likewise, testing positive doesn't mean you will absolutely get breast cancer.
Having a positive result (an identified breast cancer gene) may mean that you need to have screening mammograms at a younger age (before age 40).
There are no clear-cut recommendations regarding treatment for positive genetic tests because many women with these results don't develop breast cancer. There is no right or wrong decision. Whether or not to pursue treatment at this stage is a very personal decision that you have to make carefully based on your risk and preventative options.
At this stage, it is important that you think about breast cancer prevention. Experts suggest that consuming antioxidants (found in fresh fruit and vegetables), avoiding preservatives, and not smoking can decrease your risk of all cancers.
Specific considerations for breast cancer prevention:
Ovarian cancer occurs in roughly 1.3% of women in the general population. For those with BRCA1 mutations, 39% are expected to develop ovarian cancer, while 11 to 17% of those with a BRCA2 mutation will develop the disease.
There are other cancers that can be associated with BRCA mutations as well, such as prostate cancer, pancreatic cancer, and lung cancer.
If you or a relative have tested positive, you may become overwhelmed with worry about breast cancer. This reaction is not usual, but you owe it to yourself to sort out your feelings about the issue. If you are pre-occupied with the risk of breast cancer, it can help to talk to a therapist who can listen to you and provide you with strategies to cope with your feelings and apprehensions.
Once you have your BRCA results, you can work with your healthcare provider and genetic counselor to decide on your next steps, which will include breast cancer screening and potentially other therapies, such as hormone therapy or surgery. Voice your concerns. Ask your questions. It's important that you feel confident about what you do following BRCA testing.